Osteoarthritis, also known as degenerative joint disease, is the most common form of arthritis in the United States and it affects more than 40 million Americans. Osteoarthritis has been typically thought of as a “wear-and-tear” condition that primarily affects the joints of elderly individuals. However, osteoarthritis can occur in younger men and women, especially if prior joint damage occurred through trauma or overuse.
Typically, osteoarthritis affects the weight-bearing joints such as the hip, knee, lower back, and neck. However, osteoarthritis also commonly affects joints that are prone to overuse, such as the finger joints and the base of the thumb. The first stage of osteoarthritis is characterized by the loss of cartilage, which in turn leads to decreased cushioning of the joint and eventual bone-on-bone rubbing that causes pain.
Warning signs to alert a patient of possible degenerative joint disease include:
• Relatives with osteoarthritis
• History of injury to a joint
• History of surgery on a weight bearing joint
• Obesity
• Pain, stiffness or swelling, especially after inactivity
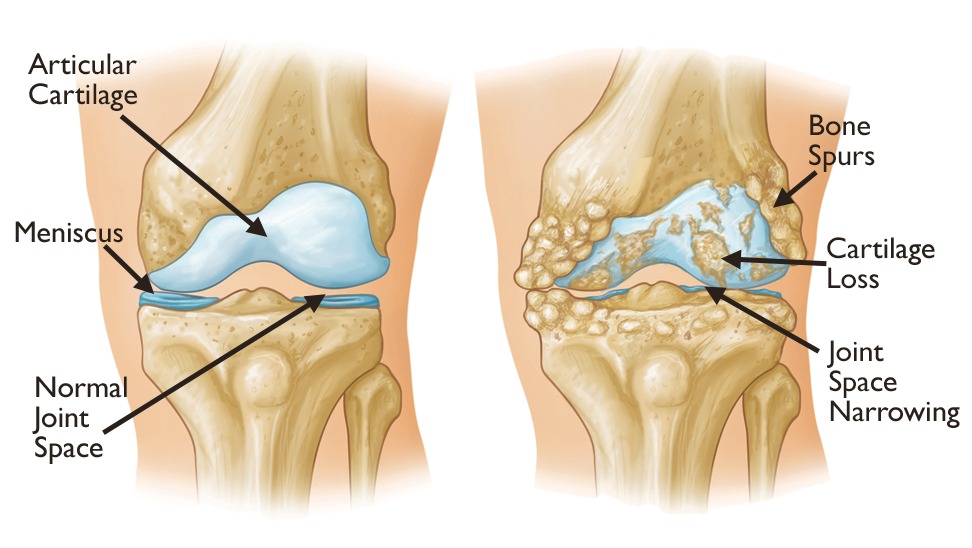
In the process of trying to heal the damage, the cartilage cells, known as chondrocytes, attempt to repair the cartilage loss. This repair is done haphazardly and does not compare in strength or elasticity with the original cartilage. If untreated, there can be ongoing thinning of cartilage and overgrowth of bone, called bone spurs. Eventually, the cartilage that cushions the ends of the bones can be completely gone. This late stage of osteoarthritis usually causes pain with mobility and the joint may develop deformities.
There is a strong genetic influence in developing osteoarthritis, especially among females. Trauma or surgery to the joint cartilage may also be a risk factor for the development of early osteoarthritis. For example, surgical treatments, like a complete meniscectomy, or removal of the meniscus from the knee, can lead to early osteoarthritis. In addition, obesity can predispose an individual to early development of osteoarthritis in the knees, hips, and spine.
Symptoms
Osteoarthritis can present with the following symptoms:
• Mild to severe pain in a joint, especially after overuse or long periods of inactivity, such as sitting or sleeping
• A grinding or grating sensation in the joint
• Swelling, stiffness, and limited movement of the joint, especially in the mornings
• Weakness in muscles around the joint caused by lack of use
• Deformity of the joint
Because osteoarthritis is so common and leads to widespread pain and disability, early intervention is key. Treatment goals include control of symptoms, such as pain, as well as maintaining function of the affected joint.
Sometimes joints can acutely “flare” with increased swelling and pain. This may be a sign that the condition is worsening, or possibly another arthritic condition is occurring at the same time, such as gout, pseudogout or a superimposed joint infection. Regardless of the cause, worsening symptoms require prompt attention by a physician experienced in treating arthritis.
Diagnosis & Treatment
If you are referred to a rheumatologist for evaluation and treatment of possible osteoarthritis, a history and complete physical exam will be performed to determine the cause of the problem. X-rays will usually be needed to confirm the type of arthritis and its severity. Fluid may be withdrawn from joints with excessive swelling to help establish a diagnosis. Sometimes more sophisticated tests, like an MRI, may be needed.
Treatment is multifaceted to decrease pain, improve joint mobility and prevent future progression of osteoarthritis. The following interventions may be used:
• Weight reduction
• Physical therapy evaluation and treatment
• An ongoing exercise program to conserve joint mobility and improve muscle strength
• Nutritional supplementation
• Pain and anti-inflammatory medications
• Joint injections to control pain
By instituting treatment with multiple different modalities, the ability to continue an active lifestyle with the lowest level of discomfort is possible. In more severe cases, surgery may be an option to restore function and improve pain. If there is osteoarthritis in the hip or the knee, a joint replacement may be necessary if symptoms are severe enough.

